Needlesticks
If you have a needlestick on the job, please follow the steps below:
- Immediately wash the affected area with copious soap and water.
- Inform the charge nurse and nurse supervisor
If at Parkland:
- Go to the paging directory
- Search the "On call" tab for "needlestick.”
- Page the first call for Needlestick and Splash exposure.
If at Clements:
- Page the Occupational Health Nurse on the 24‐hour Exposure Pager at (214)588‐6263.
If at the VA:
- Notify your immediate supervisor (Chief)/attending on service.
- Where to go:
- Regular business hours: Employee/Occupational Health Clinic (EOHU, Clinic 15)
- Afterhours/Weekends/Holidays: Present to the Emergency Department. It is not necessary to check in like a patient. Go to the main provider workstation and inform one of the providers that you had a needlestick injury and need to complete the protocol. They will enlist help from the appropriate nursing staff.
- There is a binder for logging needlestick injuries. In the binder you will be assigned a number (to protect anonymity of your labs and other data). You will receive a three-page packet of paperwork. The ED nursing staff is responsible for locating the binder and the packet of paperwork.
- The first page is to be completely filled out by the person with the needlestick injury. The second page should be filled out together by the ED physician and person with the needlestick injury. To complete this paperwork, you will need basic information like the source patient’s name and the last 4 digits of their SSN. The second page of the form asks for additional information about the source patient that may require further EMR review (HIV, Hep B, and Hep C status). If the patient consents, serologies for these bloodborne diseases will need to be ordered. Note that the order should be from a provider that is not directly responsible in the patient’s care (e.g., a provider not from the primary team). This could be the ED physician or a physician in the employee health office. If there is concern for acute HIV or hepatitis infection, note that it may be necessary for viral loads to be measured as well in the case that screening antibodies have not yet turned positive. While this should not be your responsibility, you should make sure that someone orders the appropriate studies on the patient (if the patient consents) as this has been an issue in the past (with no labs ordered or possibly an incomplete set of labs).
- After completing this paperwork, you will have your own labs drawn. You do not need to be checked in as a patient, but your labs will need to be collected and sent to the lab. Part of the protocol involves the ED staff calling or directly communicating with the lab about your lab studies because they will not be ordered in CPRS and may not have traditional labels (your needlestick ID number from step 2 is the identifier).
- After completing the paperwork and having labs drawn, you should be offered HIV post-exposure prophylaxis. Verbal consent is all that is required to receive the medication. Again, you should not need to be checked in as a patient, sign paperwork regarding payment/reimbursement for medical care, or have any orders placed in CPRS. (They may require identifying details to put you in the system so that they can remove the medication from the machine but that is all). Post-exposure prophylaxis will be in a bag and contain a three-day supply of the medications.
- For all needlestick injuries, the ED physician is responsible for paging the ID attending on call to inform of the event and steps taken.
- After completing paperwork, having labs drawn, receiving post-exposure prophylaxis (if desired), and notification of the ID physician on call, your action steps in the ED are complete.
- You should follow-up in the Employee Health Clinic (Clinic #15) within 24-48 hours of exposure (or sooner if recommended) for follow-up of lab results, any additional exposure counseling, and dispensation of addition post-exposure prophylaxis medication (if applicable). The hours for employee health are as follows: Mon/Wed/Fri 7:30AM-4:00PM and Tues/Thurs 6:00AM-5:30PM.
Please contact the Chiefs at any hour of the day or night if you have any questions.
I Feel Unwell While at Work
If you begin to feel sick at work and worry that you won’t be able to adequately care for patients, please go through the following process:
- If you have URI symptoms, put on a mask
- Ensure your team can cover your pager for you while you step out of the work room
- Call the Chief-on-Call
- If you and the Chief-on-Call decide that you cannot work anymore, be sure to:
- Notify your team that you are leaving work
- Unassign yourself as first call and ensure another team member is assigned in your place
- Run the list with your team over the phone after you get home safely
It is Unsafe for Me to Drive Home Safely
Whether the roads are too icy, or you are too tired to drive after a long night on-call, the residency program wants you to get home safely.
If you are too tired to drive, it is always best to return to your call room and nap for a while after rounds. We only ask that you call EVS if you leave the call room after 1:00pm and ask them to clean the room so that it is ready for your colleague that night.
If you need to call a cab/ride share, the program may be able to reimburse you for transportation. Always save itemized receipts of your trips and send them to . They will do what they can to get your transportation reimbursed, though we cannot guarantee it.
COVID-19
I’m worried I have been exposed to or have COVID myself
Parkland-paid Resident COVID Symptom/Exposure Survey
UTSW-paid Resident COVID Symptom/Exposure Survey
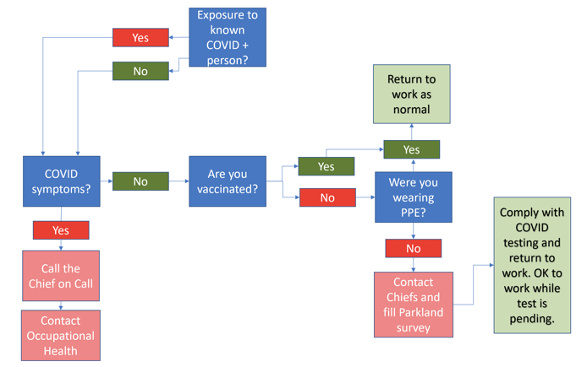
Resources for caring for patients with COVID
Additional Resources
Hospitalist Medicine COVID Central
Inpatient COVID Management (up to date as of 1/2022)
